Every minute, someone in the world experiences a stroke, an event that can instantly change a life forever. But what if you could decipher the mysterious patterns leading up to this life-altering event? Dive into the intricate world of strokes—where we unravel not just its origins but also who it targets, the silent signs it gives away, and the innovative treatments that can bring hope. Whether you’re looking to arm yourself with knowledge for a loved one’s sake or merely curious about this medical phenomenon, our in-depth exploration promises to enlighten, inform, and perhaps even inspire you to take proactive steps. Keep reading, because understanding strokes could be the very knowledge that saves a life.
What is a Stroke? An In-depth Definition
A stroke, commonly known as a brain attack, occurs when blood flow to a portion of the brain is either interrupted or reduced. This deprives brain tissue of oxygen and essential nutrients, leading to the death of brain cells within minutes. The resultant damage can have wide-ranging effects, depending on the part of the brain affected and the duration of oxygen deprivation.
Ischemic vs. Hemorrhagic Strokes: What’s the Difference?
- Ischemic Stroke: Accounting for approximately 87% of all strokes, ischemic strokes are caused by blockages or narrowing of the arteries that supply blood to the brain. This interruption often results from blood clots, either from another part of the body (embolic stroke) or ones that form in an artery that supplies blood to the brain (thrombotic stroke).
- Hemorrhagic Stroke: This type of stroke is less common but tends to be more deadly. It occurs when a blood vessel in the brain leaks or ruptures. The two main types of hemorrhagic strokes are:
- Intracerebral hemorrhage: Here, a blood vessel inside the brain ruptures, spilling blood into the surrounding brain tissue, causing damage.
- Subarachnoid hemorrhage: This is when an artery on or near the surface of the brain bursts, spilling blood between the surface of the brain and the skull.
Anatomy of a Stroke: What Happens Inside the Brain?
When a stroke occurs, the disruption of blood flow means the affected area of the brain cannot get the oxygen it requires. Brain cells, highly sensitive to lack of oxygen, start dying off almost immediately. As these cells perish, the functions they control – be it speech, mobility, memory, or other faculties – are compromised or lost.
However, it’s not just the initial event that’s concerning. The aftermath of a stroke sees a cascade of inflammatory responses and increased vulnerability in the brain, leading to secondary damage. For instance, the area immediately surrounding the stroke site, known as the ‘penumbra,’ is at risk as cells here become deprived, but not entirely without, blood flow.
Understanding this anatomy and progression of a stroke is crucial. It underscores the importance of prompt medical intervention to limit the extent of brain damage and enhance the possibility of recovery.
Who is at Risk? The Demographics of Stroke Victims
Every year, strokes affect about 700,000 globally, but not everyone faces the same level of risk. Several factors play into an individual’s susceptibility, and while some of these are modifiable, others are inherent aspects of one’s identity.
Age: A Primary Risk Factor
It’s widely acknowledged that the risk of stroke increases with age. While strokes can and do occur at any age, individuals over 65 are particularly at risk. In fact, for each decade after the age of 55, the risk of stroke doubles. This is often due to the natural wear and tear on arteries with age and the higher likelihood of having other stroke-related medical conditions in older age.
Gender Disparities: Men vs. Women
Both men and women can be victims of strokes, but their risk profiles differ:
- Men tend to have strokes at a younger age.
- Women, while generally experiencing strokes later in life, have a higher lifetime risk. This is partially because they tend to live longer than men. Additionally, certain risk factors such as migraines, taking birth control pills, pregnancy, and hormone replacement therapy can uniquely influence women’s stroke risks.

Racial and Ethnic Differences
- African Americans have a significantly higher risk of stroke than Caucasians, owing to higher incidences of high blood pressure, diabetes, and obesity.
- Hispanic Americans also face a higher stroke risk than Caucasians, with diabetes playing a significant role in this disparity.
- Asian and Pacific Islanders have shown variable risks depending on their specific ethnic backgrounds, with some studies suggesting higher hemorrhagic stroke rates in these populations.
Pre-existing Conditions Elevating Risk
Several medical conditions can significantly elevate an individual’s risk for stroke:
- High Blood Pressure (Hypertension): The leading cause of stroke, and the most significant controllable risk factor.
- Heart Diseases: Conditions like coronary artery disease, heart valve defects, and irregular heart rhythms (like atrial fibrillation) can increase the risk of clot formation.
- Diabetes: While it mainly affects blood sugar levels, diabetes also affects blood vessels, thereby increasing stroke risk.
- High Cholesterol: Excess cholesterol can lead to the formation of plaques in arteries, which can cause blood clots.
- Obesity: Being overweight contributes to other stroke risk factors like hypertension, cardiovascular disease, and diabetes.
In essence, the interplay of demographic factors and pre-existing health conditions creates a complex risk matrix for strokes. However, recognizing these factors can be the first step in personalized prevention strategies.
Understanding the Dual Dimensions of Stroke Risk: Lifestyle Choices vs. Medical Conditions
When we talk about the risk factors leading up to a stroke, it’s essential to understand that they fall broadly into two categories: lifestyle choices and pre-existing medical conditions. While medical conditions might come across as more immediate and grave, lifestyle choices can be just as influential, especially over the long term. Let’s delve deeper into these dimensions:
Lifestyle Choices: The Power and Peril of Habit
- Smoking: One of the most significant and modifiable risk factors for stroke, smoking damages the cardiovascular system in multiple ways. It narrows the arteries, increases the chances of clot formation, and reduces the amount of oxygen in the blood.
- Diet: A diet high in saturated fats, trans fats, cholesterol, and sodium can lead to arteriosclerosis (hardening of the arteries) and raise blood pressure, both major stroke risk enhancers.
- Physical Inactivity: Lack of regular exercise increases the chances of becoming overweight, developing high blood pressure, high cholesterol, diabetes, and heart disease—all contributors to stroke risk.
- Alcohol Consumption: While moderate alcohol consumption might reduce the risk of ischemic stroke to some extent, excessive drinking can elevate blood pressure, leading to hemorrhagic strokes.
- Recreational Drug Use: Drugs like cocaine and methamphetamines can cause immediate spikes in blood pressure and can damage blood vessels, increasing the risk of a stroke.
- High- Estrogen Birth Control: This is a risk, especially for those with other risk factors.
- Hormone replacement therapy: Estrogen and progesterone replacement increase a woman’s risk for stroke.

Medical Conditions: The Silent Sirens
- High Blood Pressure: As reiterated, hypertension is a prime culprit, often lurking quietly but causing damage to blood vessels and paving the way for a stroke.
- Heart Diseases: Various heart conditions, especially those that cause clot formation or irregular heartbeats, directly elevate the risk.
- Diabetes: Beyond its direct effects on blood sugar, diabetes brings with it a host of vascular complications, which means an increased risk of stroke.
- High Cholesterol: Elevated cholesterol levels lead to the buildup of plaques in arteries, narrowing them and increasing the risk of clots.
- Obstructive Sleep Apnea: This condition, characterized by interrupted breathing during sleep, has been linked to a heightened risk of stroke, possibly due to fluctuations in blood oxygen levels.
- Genetic Factors: Family history can play an important role. If a close relative, like a parent or sibling, has had a stroke, an individual’s risk might be higher.
While some risk factors like genetics or certain medical conditions might be beyond our control, many stem directly from our daily choices and habits. This highlights the importance of adopting a proactive approach towards health and well-being, empowering oneself with knowledge, and making informed decisions that can significantly reduce the risk of a stroke.
Spotting a Stroke: Signs and Symptoms to Watch Out For
Strokes can strike swiftly and, often, without warning. However, if identified early, the consequences can be significantly mitigated. Recognizing the tell-tale signs is essential, not only for potential victims but also for bystanders who might be in a position to help.
The FAST Method: A Quick Reference Guide
The FAST acronym is a simple and widely-adopted method to remember the most common symptoms of a stroke:
- Face: Ask the person to smile. Does one side of their face droop? Is it numb? A lopsided smile can be an immediate indication of a stroke.
- Arms: Instruct the individual to raise both arms. Does one arm drift downwards? Weakness or numbness in one arm can be another warning sign.
- Speech: Ask them to repeat a simple phrase. Is their speech slurred or strange? Are they unable to speak or hard to understand? This could be a symptom of stroke.
- Time: If you observe any of these signs, even if they seem to fluctuate or disappear, it’s time to call emergency services immediately. Every second counts when it comes to stroke intervention.
Other Lesser-Known But Crucial Signs:
While the FAST method is an invaluable tool, strokes can manifest in other ways too:
- Sudden Confusion: Abrupt difficulty understanding speech or sudden, unexplained disorientation.
- Trouble Seeing: This could be in one or both eyes and might manifest as blurred vision, blackened vision, or double vision.
- Difficulty Walking: A sudden dizziness, loss of coordination, or unsteadiness can indicate a stroke.
- Severe Headache: A sudden, sharp headache without a known cause, often described as the “worst headache of one’s life,” can be indicative of a hemorrhagic stroke.
- Nausea or Vomiting: While less common, unexplained nausea or vomiting, especially when combined with other symptoms, can be a sign.
- Numbness: A sudden numbness or weakness, especially on one side of the body, including the face, arm, or leg.
It’s imperative to note that these symptoms can come on suddenly and often without pain. If in doubt, it’s always better to err on the side of caution and seek medical assistance.
In raising awareness of these signs and symptoms, we can collectively improve response times and potentially save lives. Remember, in the face of a stroke, swift action can mean the difference between recovery and lasting damage.
Diagnosing a Stroke: Procedures and Tests
When an individual is suspected of having a stroke, swift and accurate diagnosis is crucial. Early detection not only facilitates timely intervention but also informs the treatment pathway, ensuring the best possible outcomes. The diagnosis of a stroke typically involves a combination of clinical assessments, imaging studies, and blood tests.
Imaging Studies: Illuminating the Brain’s Condition
- CT (Computed Tomography) Scans:
- Purpose: A CT scan can quickly visualize the brain and detect hemorrhages, tumors, and structural abnormalities. In the context of stroke, it’s often the first test done because it’s rapid and highly effective at distinguishing between ischemic and hemorrhagic strokes.
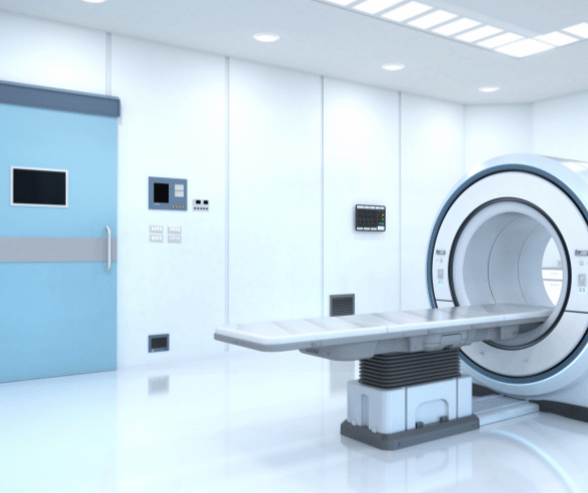
- Procedure: The patient lies on a table that slides into a doughnut-shaped machine, which captures cross-sectional images of the brain.
- Significance: While it’s adept at identifying areas of bleeding or brain injury, CT scans might not immediately detect an ischemic stroke, especially if it’s very recent.
- MRI (Magnetic Resonance Imaging):
- Purpose: An MRI provides a more detailed view of the brain compared to a CT scan. It’s especially useful for identifying ischemic strokes within the first few hours of symptom onset.
- Procedure: The patient lies inside a large cylindrical machine that employs strong magnets and radio waves to generate comprehensive images of the brain.
- Significance: MRI is particularly sensitive to changes in brain tissue and can identify areas of brain ischemia early on, making it invaluable for prompt diagnosis.
Blood Tests and Their Significance:
When someone presents with stroke-like symptoms, blood tests play a pivotal role in determining the cause and guiding treatment. Here’s what they generally look for:
- Clotting Time: Understanding how quickly the patient’s blood clots can be crucial, especially if clot-dissolving medications are being considered for treatment.
- Blood Sugar Level: Extremely high or low blood sugar can cause symptoms that resemble a stroke. It’s imperative to rule this out early in the diagnostic process.
- Electrolyte Levels: Imbalances in substances like sodium and potassium can affect brain function and may influence symptoms.
- Complete Blood Count (CBC): This test can help determine if an infection is present, as infections can sometimes exacerbate stroke symptoms or be mistaken for a stroke.
- Other Markers: Certain enzymes or proteins might be elevated in the bloodstream following a stroke. While not definitive on their own, in combination with other tests, they can provide valuable insights.
The diagnosis of a stroke is a multifaceted process. The interplay of clinical evaluations, imaging studies, and blood tests provides a holistic view of what’s happening in the patient’s brain, enabling medical professionals to intervene with the most effective treatment options.
Effective Treatment Options for Stroke Victims
The aftermath of a stroke is a critical period. Swift, targeted treatments can mean the difference between full recovery and long-term disability. Equally crucial is the long-term care and rehabilitation that supports survivors in regaining their independence and overall quality of life. Here’s a breakdown of the treatment landscape for stroke victims:
Immediate Interventions: Halting Damage and Restoring Function
Thrombolytic Drugs (Clot Busters):
- Purpose: Administered in the event of an ischemic stroke, these drugs work to dissolve the clot obstructing blood flow to the brain. The most commonly used is alteplase (tPA).
- Timing: Time is of the essence. For optimal outcomes, tPA should be given within 4.5 hours of the onset of stroke symptoms, although sooner is always better.
- Considerations: Not everyone is a candidate for clot busters. The treating physician will consider factors like the time since symptom onset, type of stroke, and other medical conditions before administering.
Surgery and Other Procedures:
- Endovascular Procedures: Doctors may thread a long catheter through an artery in the groin up to the blocked artery in the brain. Tools are sent up through the catheter to remove or break up the clot.
- Carotid Endarterectomy: In cases where the carotid arteries are narrowed, surgeons can open the carotid artery and remove atherosclerotic plaques to prevent strokes.
- Hemorrhagic Stroke Treatments: These might involve surgery to repair blood vessel abnormalities and stop bleeding. Methods include coiling (to stop blood flow to an aneurysm) or clipping (to stop blood flow to bleeding blood vessels).
Long-Term Care and Rehabilitation: Restoring Life Post-Stroke
- Physical Therapy: Helps restore physical functions such as walking, balance, and coordination. This is vital for victims who’ve lost some degree of motor function.
- Occupational Therapy: Focuses on improving daily activities such as eating, dressing, and writing. It aims to enhance independence in stroke survivors.
- Speech Therapy: For those who’ve experienced communication challenges or swallowing difficulties, this therapy works to regain these essential skills.
- Support Groups: Psychological and emotional support is crucial in the healing process. Engaging with peers who’ve undergone similar experiences can offer solace and practical advice.
- Medications: Beyond immediate treatment, stroke survivors may be prescribed medications to reduce the risk of subsequent strokes. This could include blood pressure medications, blood thinners, or cholesterol-lowering drugs.
In essence, the journey to recovery after a stroke is twofold: immediate interventions that address the urgent medical crisis and long-term rehabilitation efforts that focus on restoring the individual to their fullest potential. With the right care, many stroke survivors can lead fulfilling, independent lives post-incident.
Massage Therapy Post-Stroke: Does It Have Beneficial Effects?
The use of complementary therapies alongside traditional medical treatment often sparks interest, with massage therapy being one of the prevalent topics in the realm of stroke rehabilitation. As with any intervention, it’s crucial to weigh the benefits against potential risks, ensuring that the treatment plan is tailored to the unique needs of the stroke survivor.

Benefits of Massage Therapy for Stroke Recovery:
- Muscle Relaxation: Strokes can lead to muscle stiffness and spasticity. Massage therapy can help relax muscle tension and improve their range of motion.
- Improved Circulation: Proper massage techniques like lymphatic drainage can enhance blood flow to areas that might have reduced blood circulation post-stroke, fostering healing and nutrient distribution. [Lymph drainage]
- Pain Reduction: Some stroke survivors experience pain due to muscle stiffness, altered posture, or nerve damage. Regular massage therapy can help decrease pain.
- Stress and Anxiety Reduction: The psychological trauma following a stroke can be overwhelming. Massage therapy has been known to reduce levels of the stress hormone cortisol, promoting relaxation and well-being.
- Enhanced Body Awareness: Post-stroke, some individuals may experience neglect or reduced awareness of certain parts of their body. Swedish massage with its gentle pressure can help enhance this sense of bodily presence.
- Muscle Tone and Muscle Weakness Improvement: Massage therapy can stimulate weakened muscles post-stroke, aiding in the restoration of muscle tone and strength, and enhancing overall motor function and coordination.
Risks and Precautions to Consider:
- Sensitivity to Touch: Some stroke victims might develop heightened sensitivity. In such cases, even gentle massage might cause discomfort.
- Bone Fragility: Due to decreased mobility, there might be a risk of osteoporosis or bone fragility. It’s essential to ensure that massage doesn’t put undue pressure on fragile areas.
- Blood Pressure Fluctuations: While massage can generally be relaxing, it might lead to drops in blood pressure in some individuals. Monitoring is crucial, especially shortly after a stroke.
- Positioning Concerns: Proper positioning is vital, especially if the stroke survivor has limited mobility or paralysis.
Choosing the Right Massage Therapist:
- Specialized Training: Look for a massage practitioner with training in treating stroke patients or those with neurological conditions. They’ll be aware of the unique needs and potential complications.
- Open Communication: A good therapist will encourage open communication, ensuring the stroke survivor’s comfort and safety throughout the session.
- Consultation with Healthcare Professionals: Before beginning massage therapy, it’s essential to consult with the primary healthcare team to ensure it’s a safe and suitable option for the individual.
- Check Credentials: Ensure that the therapist is licensed or certified by a recognized body in your region.
While massage therapy can offer numerous benefits for stroke recovery, it’s paramount to approach it with caution and proper knowledge. By being informed and working in tandem with healthcare professionals, stroke survivors can harness the therapeutic potential of massage in a safe and effective manner.
Conclusion: Empowering Through Knowledge
In the complex world of medical conditions, knowledge is indeed power. Understanding strokes, from their onset and warning signs to recovery and potential complementary therapies, arms individuals with the tools they need to be proactive. Recognizing a stroke’s signs in oneself or a loved one and seeking prompt medical attention can make a profound difference in outcomes.
Moreover, leading a life informed by the risk factors and embracing habits that counteract them can significantly reduce the odds of experiencing a stroke. Prevention and early intervention are the cornerstones of a healthier, longer life.
And as we tread the path of recovery and rehabilitation, exploring holistic approaches can be invaluable. Massage therapy, for instance, has emerged as a potent ally for many stroke survivors, helping them regain not just physical wellness but also emotional balance.
If you or a loved one are on a post-stroke recovery plan, or even if you’re looking for therapeutic relaxation to combat daily stresses that can contribute to health risks, consider scheduling a session at Body Ache Escape Massage Center. Let their massage therapists skilled hands work towards your well-being, complementing your broader health strategy. [Read more about their massage therapists here]
Take action today. Your well-being is in your hands, and every proactive step, whether it’s gaining knowledge or scheduling that therapeutic massage, propels you toward a healthier future. Schedule your massage at Body Ache Escape Massage Center now.




